Definition
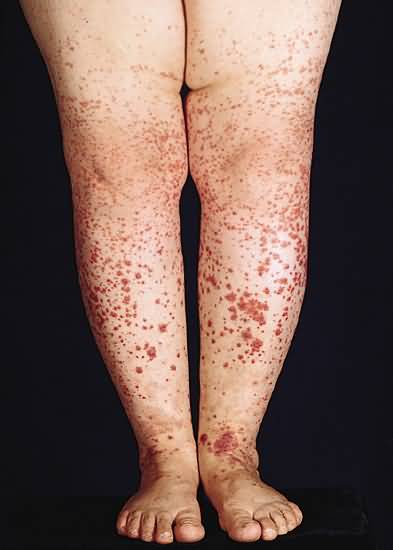
A systemic inflammatory process involving venules by deposits of fibrin within their wall in conjunction with neutrophils and nuclear “dust” of neutrophils in the dermis and, at times, the subcutaneous fat. The clinical manifestations are urticarial papules, purpuric macules, papules, pustules, vesicles, and bullae, ulcers, and scars. The effects of the vasculitis on other organs are expressed variously, e.g., by gastrointestinal pain, hematuria, and arthritis
Course
Urticarial papules are an expression uncommonly of allergic vasculitis and they tend to become purpuric rapidly. Purpuric papules, the most common presentation of allergic vasculitis, often remain just that, progressing neither to vesicles or pustules nor to ulcers. Purpuric pustules resolve as hemorrhagic crusts. Purpuric vesicles and bullae often develop a gray roof, a sign of complete necrosis of the epidermis.
As a rule, papules and blisters of allergic vasculitis continue to form, as others resolve, over time. In the case of Sch?nlein-Henoch purpura, for example, the process usually comes to a halt in weeks. In the case of allergic vasculitis that results from administration of a drug, the lesions persist as long as the drug is given; when the drug is withdrawn, new lesions cease to appear and established lesions soon disappear. A peculiar presentation of allergic vasculitis is the papules and nodules that accompany granuloma faciale/erythema elevatum diutinum. That slowly evolving, long-lasting process persists for years, devolution of it also being slow and long. In time, fibroplasia supervenes, but the lesions regress only slightly, changing in color (becoming less red or orange) more than they do in size.
In sum, depending on a variety of factors such as cause and anatomic site, and on others not yet known, allergic vasculitis may last for weeks, months, or years. Allergic vasculitis induced by a drug, such as penicillin or sulfonamide, may be relatively short lived, lasting weeks, whereas Finkelstein’s disease and Sch?nlein-Henoch purpura may persist for months, and granuloma faciale/erythema elevatum diutinum for years.
Integration: Unifying Concept
Allergic vasculitis, known by histopathologists as leukocytoclastic vasculitis, is a distinctive form of vasculitis that affects venules in a particular way. They have fibrin in their wall in the context of neutrophils and nuclear “dust” of neutrophils within the dermis especially. The findings histopathologic are the same at the outset of all expressions of allergic vasculitis, including granuloma faciale/erythema elevatum diutinum. Only after many weeks can lesions of granuloma faciale/erythema elevatum diutinum be identified with specificity for what they are by conventional microscopy, and then on the basis of nodular infiltrates in the reticular dermis made up of a mixture of inflammatory cells, namely, eosinophils, lymphocytes, and plasma cells in addition to neutrophils and nuclear “dust” of neutrophils.
Despite the fact that allergic vasculitis fundamentally is a single pathologic process, its clinical manifestations vary remarkably and range from the discrete papules of Sch?nlein-Henoch purpura, to papules arranged in the cocarde pattern of Finkelstein’s disease, to purpuric pustules, vesicles, and bullae induced by some drugs, to nodules and even tumors of granuloma faciale/erythema elevatum diutinum, the latter being different names for the same process on different anatomic sites, the face for the former and the extremities (of women mostly) for the latter.
The mechanism whereby immune complexes come to be formed is responsible for allergic vasculitis.